|
Listen to this article
|

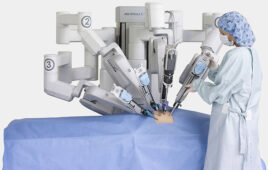
CorPath arm with extended-reach cassette. The system has been used in brain and remote surgeries. Source: Corindus
Earlier this month, a team led by Dr. Vitor Mendes Pereira at Toronto Western Hospital and Krembil Brain Institute in Canada completed the first in-human, robot-assisted stroke intervention using Corindus Inc.’s CorPath GRX system. The stent-assisted aneurysm coiling case “marked a significant milestone in interventional medicine as the first step in building towards a new treatment paradigm for patients suffering from neurovascular disease,” said the company, which is also testing remote surgeries.
“The field of neurovascular intervention is changing rapidly, but there remains a significant need to expand access to care and reduce treatment times,” stated Mark Toland, CEO of Corindus. “Implementing robotic capability for neurovascular intervention is the first step toward our vision of providing patients access to the world’s best specialists, regardless of their geographic location.”
Dr. Pereira rehearsed the procedure on a Biomex 3D-printed flow model of the specific anatomy of the patient, a 64-year-old Canadian woman. “Precision is a key element of neurovascular interventions, and it is evident to me that augmenting these delicate procedures with robotic assistance can positively impact how we treat patients,” he said.
Last month, Siemens Healthineers AG completed its acquisition of Corindus Vascular Robotics for $1.1 billion. Physicians recently used CorPath GRX, which has been submitted to the U.S. Food and Drug Administration for approval for additional procedures, in tests of remote surgeries in India.
Also last month, Dr. Ryan Madder completed 36 percutaneous coronary interventions across the U.S. over 5G networks between Waltham, Mass., and New York and San Francisco. “Our study suggests it may eventually be possible for interventional cardiologists to use robotic technology to safely and effectively perform coronary procedures from any one point to another, anywhere in the country,” he said.
Doug Teany, chief operating officer at Corindus, responded to the following questions from The Robot Report about developing CorPath GRX surgical robots and the successful procedures.
Prepping CorPath GRX for brain surgery
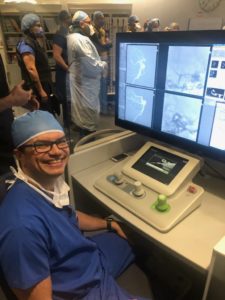
Dr. Pereira and CorPath cockpit. Source: Corindus
Was CorPath designed with the precision of brain surgery in mind, or did it require design changes?
Teany: The CorPath System is designed for precision vascular interventions. The system was originally designed and indicated for coronary peripheral interventions. To enable neurovascular interventions, we upgraded the system to accommodate small-profile devices that are used in neuro-endovascular procedures. This upgraded system is not cleared in the U.S.
We looked at stroke data from 2017 and 2018, and there were 150,000 cases addressable by interventional techniques, where the occlusion and blood vessels were large enough. However, only 5% to 7% of patients get to the right hospital in time. Remote surgeries with robotics could change that percentage to 80% to 90%.
We have an iterative product-development framework, and we’re working on appropriate capabilities for commercializing the core product. We’ve made a lot of technical progress studying force sensing, 3D reconstruction capabilities, and robotics actuation. We’re also working on hazard analysis because we understand that the clinical workflow will change.
How does telesurgery affect the doctor and patients’ experience of preparing for remote surgeries?
Teany: Telesurgery or tele-intervention enables physicians to project their specialized skillsets through remote robotics. When a remote procedure is performed, the physician is the only remote person.
The remainder of the team supporting the procedure — such as nurses, technicians, anesthesiologists — are in the room with the patient. This team completes its duties as usual, while [also] preparing the robotic system and associated devices for the remote physician to operate. The physician orchestrates team collaboration and procedure flow through an audio and visual telepresence system and performs the procedure robotically from their location.
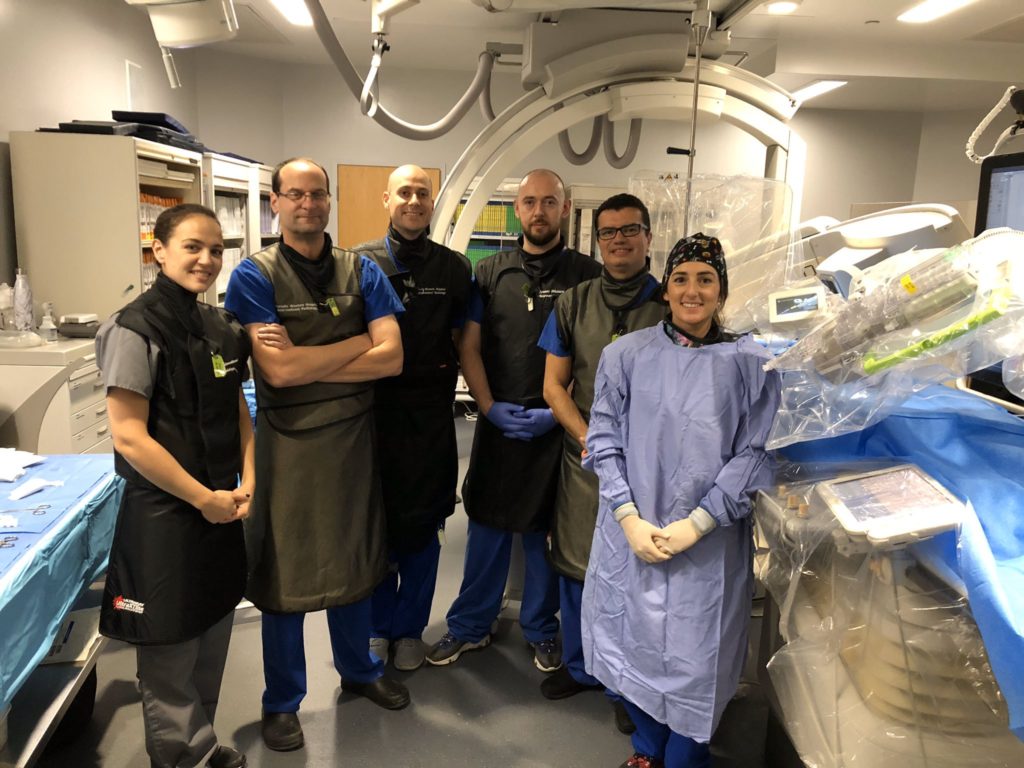
Dr. Pereira (second from right) and the team that worked on the successful procedure with CorPath GRX. Source: Corindus
From a patient perspective, there is no specific experience change for the procedure. However, patients could access care more readily with robotic systems if there is not a specialized physician at their local hospitals.
How would remote surgeries increase productivity?
Teany: A tele-intervention network could enable a more efficient system of care by connecting highly skilled specialists with patients who may be geographically limited from receiving timely care — or any care at all. This would allow highly trained physicians to improve their capabilities to treat more patients, ultimately delivering care more efficiently.
Proving the potential of remote surgeries
What were the challenges posed by the transcontinental distance or the number of remote surgeries in the 5G trials?
Teany: Previous remote studies have been performed on simulators up to 100 miles away and on patients 20 miles away. These previous experiences were very positive, with low network latencies that enable technical and procedural success.
It is important to note, with all other parameters equal, network latencies are directly impacted by signal distance travelled. During the multi-city, transcontinental study, we first doubled our remote distance from our previous maximum distance of 100 miles — performing procedures in New York 200 miles away — and then we increased the distance 30 times from our previous maximum distance, performing procedures in San Francisco 3,000 miles away.
The type of network and latency performance we would experience was unknown. We also did not know if over such distances, we would need dedicated network lines to ensure acceptable latency performance. The exciting learnings from the study showed that all connection types, up to 3,000 miles away, yielded excellent latency figures and enabled 100% success for all procedures with imperceptible latency to the operator. Most exciting about this outcome is that 3,000-mile procedures are feasible with current public Internet infrastructure.
What technologies for remote surgeries still need work?
Teany: From a feasibility standpoint, we have made significant progress to demonstrate our remote technology over short and long distances. We still have additional work to take our remote technology through the product-development process, including refining our remote product requirements and defining how to operationalize the product.
5G and remote surgeries
How did Corindus‘ 5G-enabled simulated procedures compare with those conducted over fiber or the commercial Internet?
Teany: All simulated treatments, across all connection types, were completed successfully and had low latencies that were imperceptible to the operator. The direct-fiber connection provided a dedicated connection without additional network traffic.
The 5G and public Internet connections included other network traffic. However, despite this additional traffic, there were not perceivable latency differences to the operator.
Surgeons in China have performed telesurgery over 5G on human subjects — when can we expect that in the U.S.?
Teany: We believe tele-robotics has the potential to provide patients suffering from emergent events, such as heart attack and stroke, timely and specialized care, no matter their geographic location within the U.S.
Although we have proven the feasibility of remote intervention, there is still quite a bit of heavy lifting to do in order to develop, build out, and operationalize remote robotics, and exact timing in the U.S. cannot be guaranteed.





Tell Us What You Think!