|
Listen to this article
|

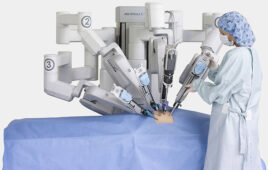
Dr. Tejas Patel conducts a telesurgery via a CorPath robotic system. Source. Dr. Patel, via Twitter
Two doctors in India this month published the results of five telesurgery procedures conducted in India via Corindus Vascular Robotics Inc.’s CorPath platform. The successful operations demonstrate an advance in the treatment of heart attack and stroke with remote, robot-assisted surgery.
The paper, “Long-Distance Tele-Robotic-Assisted Percutaneous Coronary Intervention: A First of In-Human Experience,” was released in EClinicalMedicine, which is published by respected medical journal The Lancet.
The five patients underwent elective percutaneous coronary interventions (PCI) the Apex Heart Institute in Ahmedabad, India, about 32km (20 mi.) from Dr. Tejas Patel, who was at the Swaminarayan Akshardham Temple in Gandhinagar, India.
Dr. Patel is chairman and chief interventional cardiologist of the Apex Heart Institute, and his partner, Dr. Sanjay Shah, was with each patient at the institute.
“The success of this study paves the way for large-scale, long-distance telerobotic platforms across the globe,” stated Mark Toland, president and CEO of Waltham, Mass.-based Corindus Vascular Robotics, which was recently acquired by Siemens Medical Solutions. “While remote robotic procedures are still in the early stages of development, it is clear we are on track to expand patients’ access to care, while reducing their time to treatment.”
Dr. Patel and Dr. Ryan Madder, a cardiologist in Michigan, responded to the following questions from The Robot Report about robot-assisted remote surgery, as well as its prospects in the U.S.:
Pioneering telesurgery in India
How did you become aware of Corindus’ CorPath surgical platform?
Dr. Patel: In January 2017, Riyaz Desai, who is handling the Indian operation of CorPath, introduced me to this technology. In the subsequent month, I was in New York at the Mount Sinai Interventional Cardiology Course, and I had a good discussion.
In a subsequent visit, I saw one robotic PCI case done by Dr. Manish Parikh at Colombia Presbyterian Hospital, and I was convinced about testing this technology at Apex Heart Institute. In December 2017, CorPath was installed at Apex, and we did the first [telesurgery PCI]. This was the first installation in the world outside the U.S.
Explain the procedures and how you prepared:
Dr. Patel: It was once-in-a-lifetime experience for me. There was tremendous pressure on me and my team to perform well and on logistics, including high-speed Internet. We cleared the project with the institutional review board of Apex Heart Institute and notified DCGI, the Indian equivalent of the U.S. FDA.
We lined up five cases and explained the details of the projects to all the patients. I was sitting at Akshardham on the console, and my team led by Dr. Shah was at Apex cath lab with the patients. Everything went on very smoothly, and I felt as if I was working on the patient in my lab. There was a tremendous sense of fulfillment, as India was on the record for a first in-human intervention project in medical field.
What aspects of telesurgery need to improve?
Dr. Patel: This technology has a very bright future. After incorporation of more and more artificial intelligence, the technology will make the interventions simpler and simpler. There will be less and less scope for human errors.
Once telerobotic stenting standardizes, the distance between a cardiologist and the patient will not matter. Sitting anywhere in the world, a cardiologist will be able to fix a patient’s blockages using CorPath.
What feedback did you have for Corindus after the remote cases?
Dr. Patel: All five cases went flawlessly. However, it was first-in-human study, hence as per the protocol, we chose relatively straightforward lesions.
With further refinement of this technology and incorporation of AI, we should be able to address more and more difficult cases remotely. I am dreaming of a remote console in size of a briefcase that can easily be carried by an interventional cardiologist or an interventional neuro-radiologist who can perform remote PCI or remote stroke management sitting in any corner of the world.
How much training did it require for use? Did you need to prepare your staff?
Dr. Patel: My lab crew, headed by Yash Soni, is very competent and extremely enthusiastic to adopt to any new technology. It was matter of only 10 robotic cases for them to surmount their learning curve. Nowadays, they take less than one minute to prepare the robot.
I am very thankful to Joe Aquilina of Corindus for his time and energy in training my crew. My message to any medical center adopting robotic PCI is, “Just do it!”

The Robot Report is launching the Healthcare Robotics Engineering Forum, which will be on Dec. 9-10 in Santa Clara, Calif. The conference and expo will focus on improving the design, development and manufacture of next-generation healthcare robots. Learn more about the Healthcare Robotics Engineering Forum, and registration will be open soon.
Prospects for robot-assisted remote surgery in the U.S.
What is your experience with Corindus’ CorPath system?
Dr. Madder: We installed our first CorPath system for performing robotic PCI in our cath lab in March 2014. We’ve now been doing robotic PCI procedures in our cath lab for over five years.
What sorts of procedures in the U.S. are best suited for telesurgery? How can long-distance surgery save lives?
Dr. Madder: This has not yet been determined. However, there is considerable interest in studying the ability of robotic telestenting to overcome existing barriers to PCI access, particularly in rural areas.
It has been estimated that in some rural states in the U.S., 50% of the population can reach a PCI-capable hospital within 60 minutes. This creates major difficulties for patients suffering a myocardial infarction wherein time to emergent PCI is directly linked to patient outcomes. In such situations, delays in PCI result in higher mortality, greater infarct size, and an increased risk of future congestive heart failure.
Telestenting may have the potential to eliminate the geographic barriers to PCI access and improve patient outcomes. In a similar fashion, remote robotic procedures also have tremendous potential for treating patients with acute stroke, where delays in care translate to a greater likelihood of long-term disability.
We’ve heard about “democratization of care” — what does that really mean? How much training and expertise are needed for telesurgery?
Dr. Madder: One of the barriers to implementing robotic telestenting in clinical practice is the need to have an operator with the patient who is capable of obtaining vascular access, seating a guide catheter into the coronary artery, and managing complications.
In my opinion, these tasks do not necessarily need to be performed by an interventional cardiologist, but they could be performed by other physicians or physician assistants who could be trained to perform the tasks.
Researchers in China recently announced multiple procedures conducted via 5G — what are your thoughts on that technology?
Dr. Madder: We have performed some preliminary studies investigating the ability of wireless 5G networks to support robotic telestenting and the initial results have been promising. Owing to its low latency and high bandwidth, 5G technology should be further explored as a means of supporting remote robotic medical procedures.
How much of a hurdle are costs and getting insurance reimbursements?
Dr. Madder: These issues have not yet been adequately investigated.
How long do you think it will take for telesurgery to be mature enough to be available, and how quickly do you expect adoption to be?
Dr. Madder: Although telestenting in the coronary arteries has been shown to be feasible over distances of more than 100 miles in an animal model and in humans over a distance of 20 miles, considerable research still needs to be performed before telestenting in the coronary arteries becomes widely clinically available.
Studies are needed to further explore the safety and clinical outcomes associated with telestenting, as well as to characterize the network requirements to optimally support it.





A great paper and an interesting discussion. I am very proud to see how the company I founded and the first 20 patients we published in 2007 made an impact on remote robotics.