Robots are making their way into operating rooms around the world, acting as extensions of the surgeon. Intuitive Surgical, a mainstay in the robotic-assisted surgery field, has positioned its technologies as helping surgeons boost their performance and offer minimally-invasive options to patients.
The company’s chief medical officer, Dr. Myriam Curet, shared her experience as a surgeon and as a medtech executive at DeviceTalks Minnesota 2018, the premier industry event for the medtech community produced by The Robot Report sister publication MassDevice.
Dr. Curet talked about the increased role data will play in robotic-assisted surgery, retraining surgeons, and other surgical procedures Intuitive Surgical is contemplating. Watch the interview in the video above and see the transcript below.
Before Intuitive Surgical, you were training as a surgeon. Can you tell us a little bit about what got you interested in pursuing surgery?
I actually went to medical school expecting to be a primary care physician taking care of inner-city patients who had problems with access to medical care. And what I found, actually, was I was not patient enough to be a good primary care physician. If a patient came into me and said, “I’m short of breath,” I was going to say, “well, lose some weight and stop smoking,” instead of really understanding what the issues were in helping them.
But compared to the surgeons that I trained with, I was really patient. I liked the immediate gratification, and I liked the hands-on part of it. And so I did a general surgery residency and I did that at the time that laparoscopy came out. I hadn’t learned that in my residency program. I was working for the Indian Health Service at the time.

Dr. Myriam Curet, chief medical officer, Intuitive Surgical.
I went back and I did a fellowship in order to learn laparoscopic surgery. And that’s where my clinical career began. I ended up at Stanford on faculty there and was running the bariatric surgery program, doing a lot of laparoscopic surgery on morbidly obese patients, which was very hard for me physically. They have a very thick abdominal wall. You’re having to really move the instruments against a lot of resistance. I found that, ergonomically, it really took a toll on me.
I’ve always been in academic medicine, so I’m always teaching and learning. Laparoscopic bariatric surgery is actually really hard because the suturing you do. It was a very difficult time to be a patient or surgeon at Stanford because you had new trainees coming in. And that was actually how I started using the da Vinci system in my clinical practice. Both it helped ergonomically because I didn’t have all that pressure on me of moving the abdominal wall. But it was also much easier to teach fellows and residents how to suture using the system rather than doing it laparoscopically. And that’s how I first started using the system and first got introduced to Intuitive Surgical.
How did you get involved with Intuitive Surgical?
There was a woman by the name of Catherine Mohr. I believe she’s spoken here before, so you all may have heard of her. She was actually a medical student at Stanford, but was also working for industry looking for opportunities to create new products and was in my operating room. We were talking, and she had a connection to Intuitive Surgical and she’s an engineer. So she and I actually spent some time down at the company developing the procedure, figuring out where the port should be, what the sequence of the steps were, what the instruments were.
And then Intuitive was very kind. They actually let me bring my entire operating room staff down there for two days of training. So we did it on cadavers and models. So our first time with a patient using the system in bariatric surgery, I had a really well-trained team. Our operating times for our very first robotic case were less than what our typical operating times were for a laparoscopic case.
How does Intuitive think about retraining surgeons who spend years perfecting their procedure? What do you tell patients who are wary of this technological development?
Surgeons in general are conservative. If you’ve got a routine that works well and you have good outcomes, nobody’s really willing to experiment with that in the hopes of getting better outcomes. You’ll find that many, many surgeons are not early adopters because of that reason. They will wait until the technology has been well developed. Others have experienced that there’s data out there before they will give it a try.
My own personal experience with patients was when I did my first 10 robotic cases. I told them fully that these are my first cases. This is what I’ve done to train. I brought my OR team down there and told them what I thought they would experience or not experience. I was actually really surprised, in general, patients’ vision of a robot was very positive. Their feeling was that this would only help me, and I didn’t really have any pushback.
I think sometimes surgeons, when they talk to patients, patients think that the robot is autonomous and, therefore, the robot will be doing the surgery. So it needs to be made very clear that, no, it’s a tool, it’s an enabling tool, but the surgeon is still in control, making the decisions and doing the surgery. That’s where I’ve seen a little bit of resistance from patients.
From a training perspective, I’ve seen training both from industry and also from someone who trained residents and fellows for a very long time. And it’s an interesting difference between the two. [Intuitive Surgical] feels very strongly that training on the technology itself is our responsibility. We know that system best. We know how to use it safely and effectively. But that’s only one piece of what a surgeon needs to learn to be able to use it.
So first they need to learn how to do the procedure. They’ve done that through residency and most surgeons are already doing whatever the procedure is either laparoscopically or open. They then come to [Intuitive Surgical] to get their training on the system. Then you need that piece of training of how do you use that technology in that same procedure, and that’s where I think it has to be led by other surgeons.
So whether it’s partnering with societies or whether it’s partnering with specific expert surgeons in robotic surgery to lead that. We do videos, we do case observations, we do remote mentoring, all kinds of technologies to help enable that piece of it. So it’s a continuum, and there’s a lot of people involved there. There’s a piece that we’re responsible for fully and then there’s a piece that we help enable.
What were those first 10 cases like for you?
A little nervewracking. I was getting very good outcomes with my laparoscopic bariatric surgery, and now I was trying something new. It really helped that the whole team had already been trained, so I wasn’t having to keep track of everybody’s responsibilities in the operating room. Everybody could work together as a team. But things went very smoothly and that helped me feel like, OK, this is the right way to handle it. The right things to do. Let’s now explore if we could do a little bigger patient, harder patients, and kind of start adding more complexity to what we were doing.
Can you envision robotic-assisted surgery being introduced to medical students?
I think for medical students, they have such a wide amount of information they have to get from every specialty. They have to learn about primary care medicine, pediatrics, OBGYN, surgery, that they might get a little bit of exposure to the technology on their surgery rotation. Maybe they’ll sit down or work on the simulator, but they’re not going to really use it in medical school or learn about it.
It’s really once somebody is in their residency that they’ll have an opportunity to use it in the operating room. That’s where we’ve seen really that the teaching that isn’t done by us but is done by academic medical centers, that’s where that takes place in residency and fellowship.
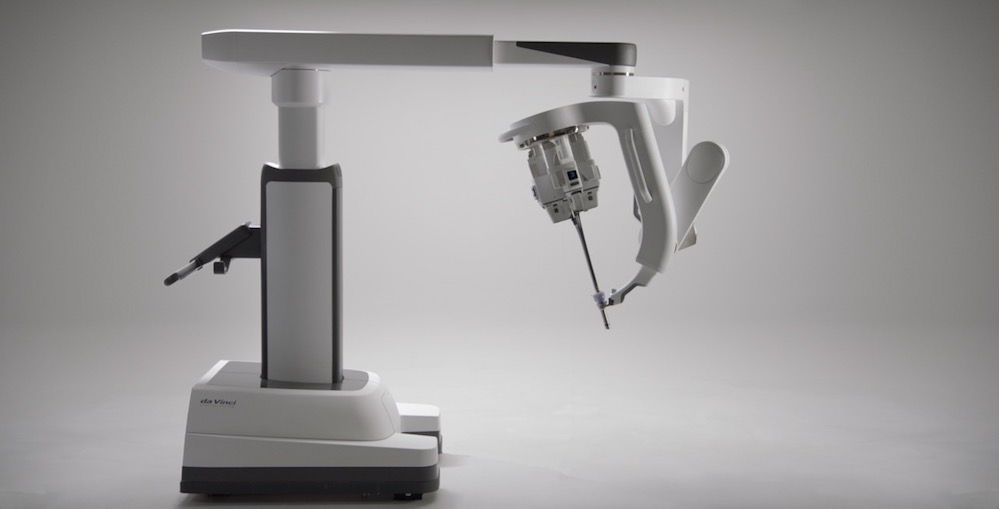
Intuitive Surgical received FDA clearance for the da Vinci SP system for urologic procedures in May 2018. (Credit: Intuitive Surgical)
What are the common concerns surgeons have with the technology?
One of the things that novice surgeons really worry about is the lack of haptics. So that sense of force feedback, which you have fully in open surgery, you lose some of that when you go to laparoscopic surgery. You’re starting to depend more on visual cues and you lose it completely when you go to robotic assisted surgery – you’re completely dependent on visual cues. We found that the expert surgeons don’t worry about that because they’ve learned how to use the visual cues, and you could actually learn them very quickly, but novice surgeons really worry about that.
Then another big difference is that with the current system, there’s four arms. So the surgeon is actually controlling the camera, two operating arms, and an assistant arm. And, again, in laparoscopic surgery you only have two hands and are only controlling two things and your assistant is controlling two others. So that aspect of how do you swap from camera movement to instrument movement or from retracting movement to operating instrument movement.
It’s very new and it’s almost a choreography that the surgeons have to learn. And the way they interact with and utilize their assistants is different than in laparoscopic or open surgery. So that’s all part of the learning continuum.
Are there certain kinds of surgery Intuitive Surgical’s technologies are well-suited for? How do you decide which to pursue or which to stave off for later?
I don’t know if any of you know the company from way back when, but the original operation that we chose to address with the initial system was actually the heart. We thought that the robotic system could change an open heart surgery with the big sternotomy to a small incisions here, so tremendous value to the patient.
What we didn’t anticipate was the learning curve associated with converting open cardiac surgery to minimally-invasive cardiac surgery and the very little leeway there was for that learning curve because you don’t want to be on pump for too long. And a surgery urologist was watching a cardiac surgeon do a robotic cardiac surgery and he thought, you know, I could use this for the prostate, which was really only done open. He was the one who came to us and said we think there’s value here.
So we aimed for the heart and ended up down in the prostate. Occasionally we have found procedures where we think there’s value and then our customers have agreed. But often it’s driven by the customer themselves who say we think there’s value in this procedure. And it was a procedure really hadn’t thought about before. So we listen very, very carefully to our customers and watch what they’re doing and have them come in for labs and have showed them our new technology to get ideas from them so that it’s a collaborative development.
Hw often does a provider or a customer suggest potential procedures?
It happens all the time. Surgeons think about things we’ve never even thought about, things that can’t be done with current open or minimally-invasive techniques. There’s people in the company who take in those kinds of calls. They get 20-30 emails or phone calls about that almost every day.
Are there certain technologies you see helping advance robotic-assisted surgery?
The wonderful thing about robotic-assisted surgery is we’ve basically put a computer between the surgeon and the patient, which is going to enable all kinds of things that aren’t possible with open or laparoscopic surgery.
So one obvious one is vision. So can you use information to see things in other wavelengths that the surgeon can’t see with white light? I do a fair amount of laparoscopic cystectomies and we use white light to visualize the common bile duct. We can now use ICG with a special infrared imaging to see the bile duct long before we have to put any clips or cut it. Could you see cancer cells? Could you see nerve cells? Would that help you remove the cancer more fully while still saving the structures that you want to keep?
Can you take an MRI or CT scan of the patient’s pathology and be able to overlay that during the surgery to help guide the surgeon to, again, make sure that all of the tumors removed and the important structures are left behind.
Then I think there’s a tremendous amount of data that we can get from the system itself that can be fed back to the surgeon and to the OR team to help them make interoperative decisions. I think we’re really at the very beginning of that journey in terms of the additional technologies that can be used to give more information to the surgeon and the OR team to help them get even better outcomes.

Sarah Faulkner (left), associate editor of MassDevice, and Dr. Myriam Curet, CMO, Intuitive Surgical, at DeviceTalks West 2018.
How does going from being a disruptor and a young company to a mainstay in the industry change your thinking about where the company is headed?
Being innovative and being a disruptor is really in our DNA. Our leaders in our company, our CEO, our chief operating officer, our chief commercial officer, have been there almost from the beginning. I think they’re employees number seven and nine. So it’s very ingrained in the company, and there’s a lot of support for R&D and a lot of support for innovation. I think we’ll always maintain that.
We do have to look at the market differently now because of competition. I personally, both as a surgeon and as the CMO, think it’s been fantastic that competition has come in. I think it validates the technology, it validates that there is a future in robotic-assisted surgery, and I think it will stimulate all of us to be more innovative and to kind of keep thinking outside the box and seeing how else we can bring value to surgeons.
We’re keeping track of what competitors are doing. We’re continuing to innovate in product, but we’re also innovating in terms of what we call the ecosystem, in terms of how can we help train surgeons better. How can we help train our staff better? How can we use analytics to help our customers better? It’s stimulated us and challenged us to be creative and innovative beyond just the platform and the instrument.
Can you expand a little bit into how you see analytics shaping your business?
I think there’s a role for analytics in various ways. I think we use analytics right now to talk with customers about how to build a very cost-efficient and quality-efficient robotics program. We can show them how they’re performing compared to their peers, help them identify best practices, and then keep giving them back the information that shows whether they’re meeting the standards that they want to meet or not.
We can also use analytics in the operating room. We can capture movements of the instruments at certain ports of the operation that are different than how an expert would do it. We can give that information back to the surgeon, or we’re exploring how to give that information back to the surgeon, to help him or her be as efficient and as safe as possible during that procedure. We’re really investing a lot in exploring how these analytics can be used kind of throughout the continuum of our relationship with customers.
You’re still in the OR every once in a while and you’re helping to guide this company. How has that perspective helped Intuitive stay in touch with what it’s customers want?
It’s very interesting using our technology in our labs as the chief medical officer and then using it as a surgeon in my operating room. I see it differently. What I want from it or need from it or what I notice is very different. And so it’s actually been very, very helpful for me to understand what our customers need and want, not just from what they say, but from what I experienced as a customer. I think that’s been really valuable to me in terms of giving feedback to our engineers, giving feedback to our marketing people.
In my academic career, my focus was really surgical education. I’m passionate about it and that’s how I actually got promoted. So the ability to now come and work with a global group of people who share that same passion around surgical education and training where we can try new technologies and novel ways of training and getting learning out of the operating room is very synergistic with what I do as a teacher at Stanford as well as what I’m trying to do as a chief medical officer at Intuitive Surgical.
I think there’s a shift among the industry and also at FDA that we’ve noticed that they’re really interested in companies gathering up real-world evidence and also finding out what patients want from the system. How is Intuitive incorporating those practices and do you see us shifting away from the randomized control trials (RCTs) and really putting our focus on the real world-evidence in the patient preference?
I think that transition started several years ago and even in Pharma not just in medical device industry. RCTs are the gold standard, but there are limitations to their generalizability. If you as a doctor have a patient that meets those exact inclusion and exclusion criteria, great. You can use those results to help you decide what the treatment should be for your patient.
But if you have a patient that doesn’t meet those inclusion/exclusion criteria, then that RCT really doesn’t help you decide how to treat that patient. And the complexity when you look at a medical is even more because you have to deal with the equipoise issue and you have to deal with the variability and surgeons abilities. My ability to do a gallbladder is going to be very different than your ability to do a gallbladder and, therefore, whether you should be doing it open, laparoscopically or robotic, it’ll be different than the decision that I would make.
We’ve actually tried multiple times to have RCTs to sponsor RCTs. And in our discussion with surgeons over and over and over, surgeons who use the robotic system will not randomize their patients to a laparoscopic or open approach. They think it’s an inferior approach. The surgeons who do laparoscopic or open surgery won’t learn robotic surgery to randomize their patients. And so we end up doing registries and cohort studies, which are real world evidence.
So the vast majority of the data on Intuitive on the da Vinci products, there’s over 12,000 publications now, is real world evidence. I was very happy to see that the FDA has come to recognize the value of real-world evidence and how helpful and important it can be. So I think we are seeing that movement, and we as a company have invested very heavily in making sure that there’s sufficient real-world evidence for people to make decisions about a healthcare decisions.
Are there other sort of regulatory reimbursement trends you’re keeping a close eye on?
Our system has been used to enable MIS [minimally-invasive surgery]. So procedures that were typically done open are now being able to be done minimally invasively because of the use of the da Vinci system. And as that has happened, those procedures have migrated to the outpatient realm, which is very positive. But they couldn’t be moved beforehand because they were being done open, they couldn’t be done minimally invasively.
We’ve seen that a lot in benign procedures, but we’re also starting to see it in cancer operation. So a prostatectomy for prostate cancer, a hysterectomy for endometrial cancer, we’re starting to see more and more of those being done in an outpatient setting. So that’s one migration that we’re keeping a very, very close eye on.
Can you recall a mentor who helped advance your career and keep your passion through these two industries?
I agree completely that mentorship is really, really critical. I would say that I’ve not had one specific mentor. I’ve had a series of mentors, and I’ve learned different things from each of them, both about things I want to do and about ways that I don’t want to be.
Surgeons have had a reputation for a long time of being very impatient, very intolerant and very rude in the operating rooms. And I saw that in my residency program, and I realized that is not how I want to be. But those same surgeons had an unbelievably great relationship with their patients. So I could say that’s the piece of them that I want mentoring on because I want to have that kind of relationship with my patient, but that’s the piece I don’t want mentoring on because I don’t want to be like that.
What I’ve personally tried to do is learn a little something from all the people that I interact with. I say I really liked the way that person does that, the way that person listens, or the way that person responds when somebody disagrees, or the way that person handles that difficult situation, while also realizing there’s parts of who they are that I cannot or don’t want to be.
I think the other piece I’ve tried to do is to feel free to reach out to people that I’ve met, that I’ve really admired and not wait for them to come to me or not wait for mentoring program to be put into place. That can be very hard to do. But in general I have found that people that I admire are very open and willing to help and mentor and give advice. When I talked to women residents or young women faculty or young women engineers, I tell them to look for mentors everywhere and reach out and talk to them. You’ll find that they’re much more responsive than you might think.
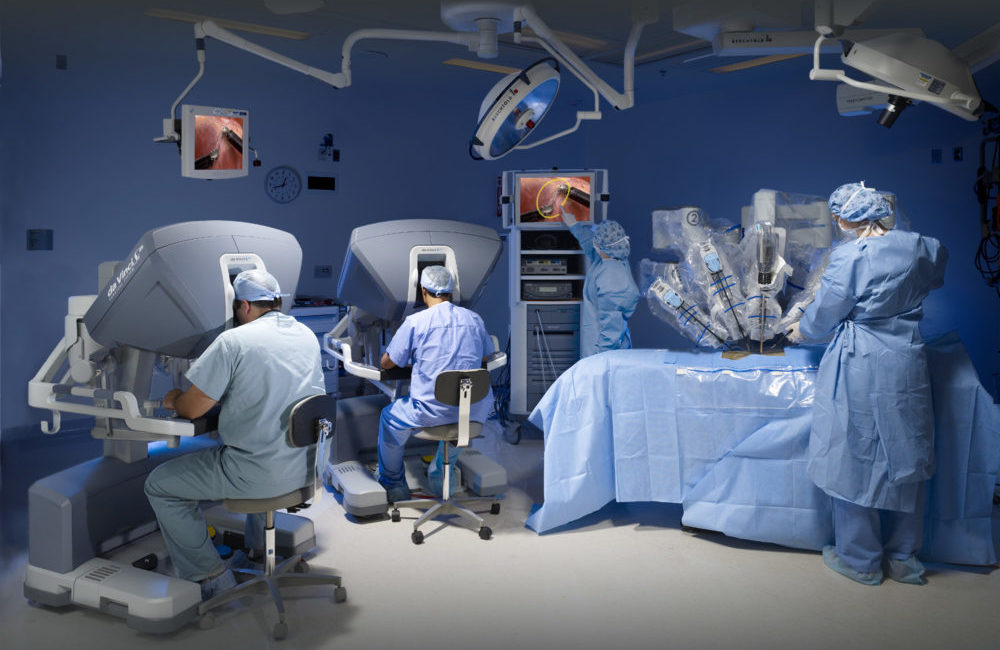
(Credit: Intuitive Surgical)
What other lessons are you now trying to impart upon surgeons?
One of the things I think that is really an issue, both in medicine and in industry, is the whole family-work balance. And I don’t have any great solutions, but I had two chairman tell me this and I really took it to heart. They would put into their schedule their family time and their personal time.
I still do this. I get my kids’ schedule at the beginning of the year and I block out the days that they don’t have school or they only have a half a day of school. And as I get close to that day, I may not be able to keep it free, but I know I won’t be able to free it up if I don’t put it into my schedule ahead of time.
So whether it’s making sure that I’m able to go to hot lunch on a weekly basis at their school or whether it’s going on a field trip, I make sure I put those things into my schedule because that’s the only way that they will be as important as all the work-related things that I have to do.
So for example, my trip here, I just got back from London Sunday and then I came here. I go back home tonight and I took tomorrow morning off to be able to take the kids to school. It allows me to have that balance and be very deliberate about it. I think that becomes easier as you get further along in your career than when you’re first starting. But if you try to do as much of that as you can throughout, I think you’re much more likely to be able to get that balance, not necessarily on a day-to-day or weekly basis, but kind of overall.
Does intuitive have internal commitments to diversity?
Diversity inclusion is very important. We think we are already a very diverse company, so it’s really more about inclusion. We do have a program where we are helping, in particular, managers understand what it means to be inclusive, what kind of language to use, how to look for situations where perhaps somebody is not feeling included, how to be able to listen to people who have a different opinion or who have a different perspective or different backgrounds. It’s something we realize that in this day and age in order to be successful as a company, you absolutely have to be committed to diversity and inclusion.
Where do you see the field of robotics surgery headed?
I really think that we’re in the infancy of what robotic-assisted surgery can do. As we look to new applications, we look at catheter-based robotics, we look at diagnostic-based robotics, we look outside of the abdomen and pelvis and thorax, we will continue to find procedures where having a computer there, having a robot there, will bring value.
I’ve seen two revolutions in my surgical lifetime: the laparoscopic revolution and now the robotic revolution. My guess is 10 or 15 years from now it will change yet again as technology continues to evolve. But really the focus is going to continue to be more minimally-invasive. The more minimally-invasive you can get, the better outcomes are for patients and the better their journey is. I think eventually we will move to a place where as many procedures as possible that can be done with the smallest incision, or no incision at all, will really be the goal for companies.
Will surgeons ever be totally removed from the process or do you always see the system as being a tool to augments their practice?
I actually think the technology to create an autonomous robot will be easy to solve. That I don’t think is the problem. I actually think the problem will be the regulatory environment. I mean to be able to prove that that is safe and effective to the FDA standards is going to be incredibly difficult. I think that’s where the bottleneck will be for autonomous robots. Whether you’ll be able to autonomize portions of it, I think that could come in my lifetime, well maybe in your lifetime, but I think that that will happen. I don’t think that’s a technology problem, I think that’s a regulatory problem.
A lot of data streams in the operating room, ability to see beyond just what can be seen with white light; trackers that are tracking the movements of the OR team to making sure they’re being as efficient as possible. Technology that allows an anticipation of what’s needed next or what’s going to be done next.
I’ve actually seen some suggestions that you could replace the scrub tech or the OR nurse with robots. I don’t know that we’ll ever get to that point. I think what you’ll see is more and more technology that is more and more enabling to allow patients to have the best possible outcomes and the best possible journey.
We don’t want technology to get in the way of human-to-human interaction. What’s the balance like there?
I think that’s where the problem is and where the tension is. I don’t know exactly how we will end up with that. I think we’ve already seen changes in that, and I think it’ll continue to evolve. I’m curious to see where it ends up.





?!? Dear People, I just had an idea about a new application of your da Vinci system of robotic surgery. That is, what if we could use this device to make a complete cure of the condition called Endometriosis that afflicts millions of women. In this medical condition, tissue that is only supposed to grow inside the woman’s uterus also grow in nearly any place outside of it, inside the pelvic or abdominal area, and can cause terrible pain when that tissue grows suddenly during her menstrual cycle. Why not use the da Vinci to remove ALL of that misplaced tissue? Well, apparently, we cannot presently, due to it being hard to detect or differentiate from the surrounding organs. SO, WHAT IF we created a special order drug, that we can inject into the bloodstream of such Endo-patients, whose only purpose is to DYE this specific type of tissue a SPECIFIC COLOR? That way, it might be able to modify this robot, with a fiberoptic micro-cable, to shine a light onto the areas it’s probing, and the robot would be able to ‘see’ the misplaced tissue, and only target its actions on the exact spots with that color. Also, it might be feasible to install a minute ‘Pac-Man’ device onto this ‘smart’ da Vinci catheter, a tiny thermal laser, that simply evaporates the unwanted tissue a tiny bit at a time, and then uses a vacuum cleaner mechanism to suck up the burned vapor? I think that there was an old cardiac artery clearing surgical device, called a ‘Fat-Shaver’, with witch heart doctors could thread up to a artery that is ‘thinned’ by Artherosclerosis plaques, and shaves that pipe-clogging stuff off the inner walls of the artery, and they retract it out with a tiny basket. If you consulted with the makers of that device, they may be able to help you perfect this new da Vinci surgery technique as well. And, don’t forget, that an established tech option with this thing, is that by adding a stainless steel construction to the business end of this special ‘smart’ catheter, we can use a strong magneto manipulate it precisely from outside of the patient’s body. Although, they already use open-abdomen surgery to help Endo-patients, a robot, which is tireless and also remotely controlled by IBM’s Watson or something, might be able to do these procedures, with a LOT less problems and also enable a permanent solutions. This treatment could entail pain, of course, but we already have painkillers so potent, that we can stop ANY pain problem easily. That covers it.